How to fix scoliosis
Here’s how to fix scoliosis when you know what’s scoliosis exactly. If you have it, you need to know who can help. By fixing it are you getting rid of curvatures forever or only dealing with pain if there is any. We’re covering it all in one go.
Scoliosis Categories
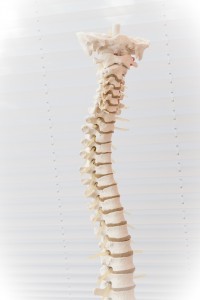
Scoliosis is any abnormal sideways curvature of the spine measuring at least 10 degrees on an x-ray. Extreme cases of scoliosis can be disabling, causing lung and heart complications. The general categories are structural scoliosis and nonstructural or functional scoliosis.
Structural vs. Nonstructural Scoliosis
Here are two general categories for scoliosis:
- Structural scoliosis is by far the most common category of scoliosis. It involves spinal rotation in addition to the side-to-side curvature of the spine. This type of scoliosis affects the spine’s structure and is considered permanent unless the spine receives treatment.
- Nonstructural scoliosis, also known as functional scoliosis, results from a temporary cause and only involves a side-to-side curvature of the spine (no spinal rotation). The spine’s structure is still normal.
When we do an orthopaedic standing exam at Susannah Makram clinics for osteopathy we are looking at the scoliosis curve in motion. If a client with nonstructural scoliosis or functional scoliosis bends forward or lies down, the scoliosis curve will likely disappear for as long as this position is held.
Structural scoliosis is typically considered more serious because it doesn’t straighten out on its own and can potentially result in more spinal deformity.
Common Causes of Nonstructural Scoliosis
While non-structural scoliosis is relatively uncommon, here are some ways it can occur:
- Muscle spasms. If a major muscle in the back starts to spasm, the spine can be pulled in one direction and a sideways curve may result.
- Difference in leg heights. This is when one leg is significantly longer than the other – either by bone length, pelvic positioning (therefore in appearance etc. In either instance a scoliosis curve may be present while standing.
- Inflammation. This is when an area of the body to one side of the spine or the other starts to become inflamed. Cupping massage with hot and cold therapy can be extremely helpful to reduce inflammation. Where present a scoliosis curve can result. Some possible extreme causes could be of inflammation can be appendicitis or pneumonia.
Scoliosis and Osteopathy
Signs of Scoliosis can include:
• Uneven musculature on one side of the spine
• Rib prominences or prominent shoulder blade, caused by rotation of the rib cage in Thoracic scoliosis (mid back)
• Uneven hips, arms (shoulders) or leg length
How to fix scoliosis that is non structural scoliosis is quite common with osteopathy. We tend to find this with muscle imbalance any way. Sometimes it’s very small and barely noticeable. You can learn about ways to maintain a better posture to keep your functional scoliosis at bay after osteopathic treatment.
Osteopathic approach to scoliosis
Osteopathy can help when looking into how to fix scoliosis. We’re asked how to fix scoliosis without surgery often in clinic. Contact us for your healthy journey outlook for using osteopathy and exercises for scoliosis.
Treating Scoliosis at Susannah Makram Clinics – osteopathy and Scoliosis.
How much does your scoliosis affect your day to day movements and functions? Osteopathy with Susannah can help by reducing inflammation often created by small tears in overused muscle fibres with scoliosis using cupping massage combined with cyrotherapy.
Also, mobilising the thoracic spine (mid back), sternum, ribs, shoulders and associated muscles by gentle but precise traction and stretching.
Working into the fascia to stretch the diagram, and hip muscles, actively and passively to regain lost muscle memory and also lumbar spine. trying to increase the range of movement in both areas.
Reverse scoliosis with exercise
Mobilisation of the pelvis is also be necessary to aid leg length and in turn, help straighten the lower back and further up the spine. This is best when worked into day to day gym or exercise programmes of the client. At Susannah Makram Clinics we personalise dynamic movement strength training according to the client
Find out more